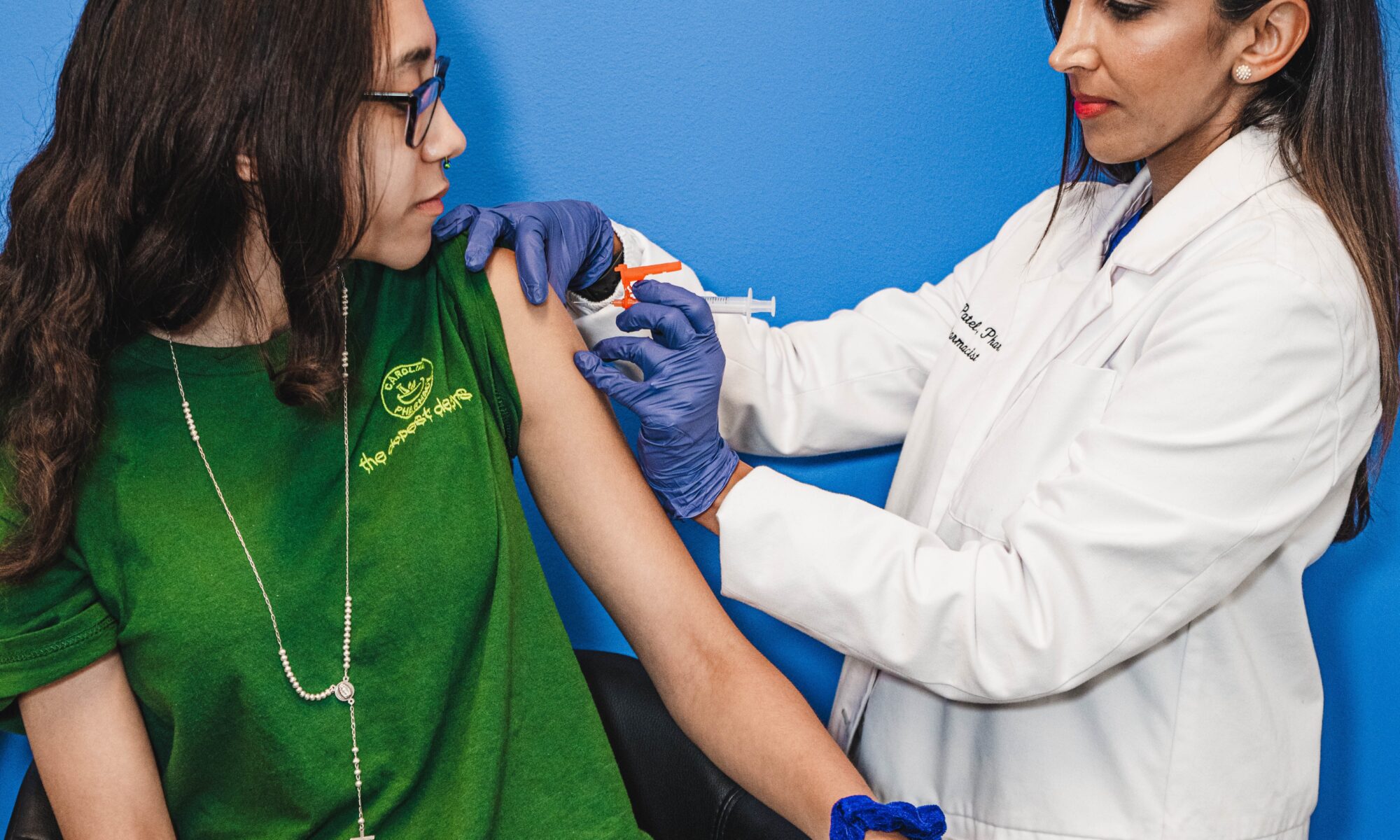
The flu virus evolves yearly, bringing new challenges to our immune systems. Getting a flu shot is a simple yet powerful step to protect yourself and those around you from this ever-changing threat. As we continue navigating the COVID-19 pandemic, our pharmacists at Carolina Pharmacy have created this post to dispel common myths and explain why getting a flu shot vaccine in Charlotte, NC, Rock Hill, and Lancaster, SC is vital for staying healthy.
Understanding the Flu Vaccine and How It Works
The flu, or influenza, is not just a bad cold. It’s a serious respiratory illness caused by influenza viruses that can lead to hospitalization and, in severe cases, death. The best defense we have is the flu vaccine.
Influenza vaccines work by imitating an infection to build immunity. When developing the annual flu vaccine, scientists cultivate viral flu particles that researchers carefully select to match the most prevalent flu strains of the year. They replicate these viral particles, kill or weaken them to inactivate them, purify them, and use them to create the influenza vaccine or “flu shot.”
Once administered, the vaccine prompts the body to produce a defensive response in the form of antibodies against the flu virus. These antibodies are primed to prevent flu infections or reduce the severity and duration of the flu if someone vaccinated gets sick with a strain not covered by the vaccine.
Debunking Myths About the Flu Shot
There are several misconceptions about flu shots. Here, we debunk some of these myths, each one backed by scientific evidence and our expert opinion:
Myth 1: The Flu Shot Can Give You the Flu
The flu shot contains inactivated viruses or a single gene from a flu virus (for the recombinant vaccine) that cannot cause illness. These components stimulate your immune system to defend against the virus. Mild symptoms after vaccination, such as low-grade fever or muscle aches, are not the flu but a sign your body is building immunity.
Myth 2: I’m Healthy; I Don’t Need A Flu Shot
While it’s great that you’re healthy, the flu can be unpredictable. Moreover, getting vaccinated is not just about protecting yourself; it’s about protecting the people around you, including those who can’t be vaccinated, such as newborns or people with severe allergies to vaccine components.
Myth 2: I Got the Flu Shot Last Year, So I’m Covered
The flu virus is constantly changing, which is why a new influenza vaccine is developed each year to match the strains predicted to be most common. Skipping a year means you won’t be protected against the current strains, putting you at the risk of contracting the virus.
Who Should Get the Flu Shot?
The Centers for Disease Control and Prevention (CDC) advises that everyone aged six months and older should receive the yearly influenza vaccine. They emphasize that this vaccination is the primary and most important measure in safeguarding against the flu virus.
Reasons to Get a Flu Shot in Charlotte, NC, Rock Hill, and Lancaster, SC
Flu shot vaccine benefits extend beyond preventing the flu itself. It lessens flu-related hospitalizations for all ages, safeguards individuals with chronic conditions like COPD, and protects pregnant women and babies from flu-related respiratory infections.
By getting vaccinated, you’re not just protecting yourself. You’re also contributing to what’s known as “herd immunity.” When a significant portion of the population is vaccinated, it’s harder for the flu to spread. This is crucial for protecting people at high risk of serious flu complications, including babies, pregnant women, seniors, and people with certain chronic health conditions.
Does the Flu Shot Help With COVID-19?
No, only a COVID shot can. Flu vaccines won’t protect you against COVID-19, but they will help reduce the overall impact of respiratory illnesses on your health and the healthcare system, ensuring the resources are available for COVID-19 patients. And yes, getting the COVID shot and flu vaccine is safe.

Protect Your Health With a Flu Shot in Charlotte, NC, Rock Hill, and Lancaster, SC
Carolina Pharmacy offers flu shot vaccines in Charlotte, NC, Rock Hill, and Lancaster, SC to help you stay on top of your health. Contact us today for more information on the influenza vaccine, COVID-19 testing or the vaccine, and practical tips to protect your health.